INJECTION ANSWERS
WHEN YOU NEED THEM
Find the information and resources to help manage your relapsing multiple sclerosis (RMS) therapy.
Preparation tips for injecting Teva's COPAXONE®:
Schedule an appointment with your healthcare provider for injection training. Even if you have used an injectable therapy before, you should be trained by a doctor or nurse before you inject COPAXONE® for the first time.
Organize your supplies. Download the Injection Guide for easy-to-reference materials you can print out to use when injecting at home or wherever is best for you. Start by placing each item you'll need on a clean, flat surface1:
-
1 COPAXONE® prefilled syringe
-
A warm compress (if you're using it)
-
An alcohol wipe
-
A dry cotton ball
-
A used-syringe disposal container
Before Injecting
When Injecting
After Injecting
-
Always wash your hands before injecting.1
-
Remember—wait 20 minutes until your prefilled syringe has reached room temperature before injecting.1
-
Some people find it helpful to use a warm compress before injecting.
-
Always use a cloth barrier between bare skin and the warm compress.
-
Do not use the warm compress in areas where sensation of temperature is impaired.
-
Alternatively, it may help to ice the site for 1 minute before cleaning the site and injecting.
-
Clean your injection site with an alcohol wipe, and make sure your skin is dry before injecting.1
-
Rotation matters. It is extremely important to rotate your injection areas (and sites within each area) to help keep your skin as healthy as possible.1
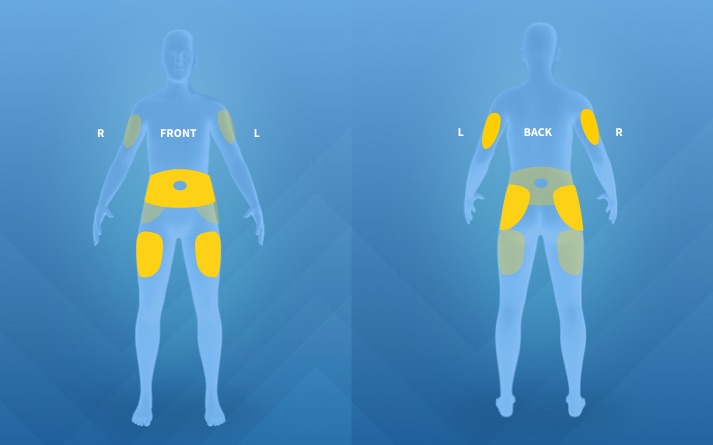
-
There are 7 injection areas to rotate between. Be sure that you do not inject in the same place (site) more than 1 time each week.1
-
Your doctor may be able to recommend other appropriate injection sites, if needed.
-
Avoid injecting into sites with birthmarks, tattoos, stretch marks and scars and/or other skin irregularities.1,2
-
If there are particles in the syringe or the solution is cloudy, do not use it.1 Report this event to the FDA by calling 1-800-FDA-1088 and to Teva by calling 888-TEVA-USA.
-
Never inject with a needle that has been dropped on the floor or has come in contact with any other surface. Start over with a new syringe.
-
Avoid hot showers or baths after you inject.
-
Do not massage the site immediately after injecting—this can damage underlying tissue. Wait at least 24 hours after injecting.2
-
Dispose of used syringes in a hard-walled plastic or disposable biohazard sharps container immediately after you inject.1
-
If you miss a dose, take your COPAXONE® as soon as you remember. If it is nearer to the time of your next scheduled dose, skip the missed dose and resume your usual dosing schedule.
-
If you have any questions about missing a dose, contact your healthcare provider for assistance.
Please read the Patient Information in the full Prescribing Information.
References:
-
COPAXONE® (glatiramer acetate injection) Current Prescribing Information Parsippany, NJ. Teva Neuroscience, Inc.
-
McEwan L, Brown J, Poirier J, et al. Best practices in skin care for the multiple sclerosis patient receiving injectable therapies. Int J MS Care. 2010;12(4):177-189. doi:10.7224/1537-2073-12.4.177
You are about to leave COPAXONE.com and enter a website operated by a third party.
Would you like to continue?
The information on this site is intended for healthcare professionals in the United States. Are you a healthcare professional in the United States?



